Myelodysplastic Syndrome: Silent Signals You Shouldn’t Ignore
Fatigue that lingers, easy bruising, or frequent infections can look like everyday issues, yet they may reflect changes in how your bone marrow makes blood cells. Myelodysplastic syndrome (MDS) is one condition that can develop quietly, so understanding subtle warning signs and risk factors can help you discuss concerns more clearly with a clinician.

Myelodysplastic syndrome represents a group of disorders where the bone marrow fails to produce enough healthy blood cells. This condition primarily affects older adults and can progress slowly over months or years. The challenge lies in recognizing symptoms that often appear harmless but may indicate a deeper problem requiring medical evaluation. Awareness of these silent signals empowers individuals to seek timely diagnosis and appropriate care.
What is Myelodysplastic Syndrome and Who is at Risk?
Myelodysplastic syndrome, commonly abbreviated as MDS, occurs when the bone marrow produces abnormal or dysfunctional blood cells. Instead of maturing properly, these cells die in the bone marrow or shortly after entering the bloodstream. This results in low counts of red blood cells, white blood cells, or platelets. The condition primarily affects people over 60 years of age, though younger individuals can develop it as well. Risk factors include previous chemotherapy or radiation treatment, exposure to certain chemicals like benzene, smoking, and genetic disorders. Some cases develop without any identifiable cause. Men are slightly more likely to develop MDS than women. Understanding these risk factors helps identify individuals who should remain vigilant about potential symptoms and maintain regular medical checkups.
What Are the Early Warning Signs of MDS?
The early symptoms of myelodysplastic syndrome often appear gradually and can be easily overlooked. Persistent fatigue that doesn’t improve with rest is one of the most common complaints. Individuals may notice unusual shortness of breath during routine activities they previously handled without difficulty. Pale skin resulting from anemia frequently accompanies these symptoms. Easy bruising or bleeding, including frequent nosebleeds or bleeding gums, may occur due to low platelet counts. Petechiae, tiny red spots under the skin caused by bleeding, sometimes appear on the lower legs. Frequent or recurring infections signal problems with white blood cell production. Some people experience unexplained weight loss or fever. Many individuals attribute these symptoms to aging, stress, or minor illnesses, delaying diagnosis. The combination of multiple symptoms or their persistence over weeks should prompt medical consultation.
Why Do These Symptoms Often Go Unnoticed?
Several factors contribute to the delayed recognition of myelodysplastic syndrome symptoms. The gradual onset means the body slowly adapts to declining blood cell counts, making changes less noticeable. Symptoms like fatigue and weakness are nonspecific and common to many conditions, leading both patients and healthcare providers to consider more common diagnoses first. Older adults, who comprise the majority of MDS cases, may dismiss symptoms as normal consequences of aging. The absence of pain in early stages means there’s no urgent alarm prompting immediate medical attention. Additionally, routine blood tests may not be performed regularly in healthy adults, allowing abnormalities to go undetected. Social factors, including limited healthcare access or reluctance to seek medical care for seemingly minor complaints, further delay diagnosis. Understanding these barriers emphasizes the importance of taking persistent symptoms seriously and advocating for thorough medical evaluation when something feels wrong.
How Does MDS Affect Your Body’s Blood Production?
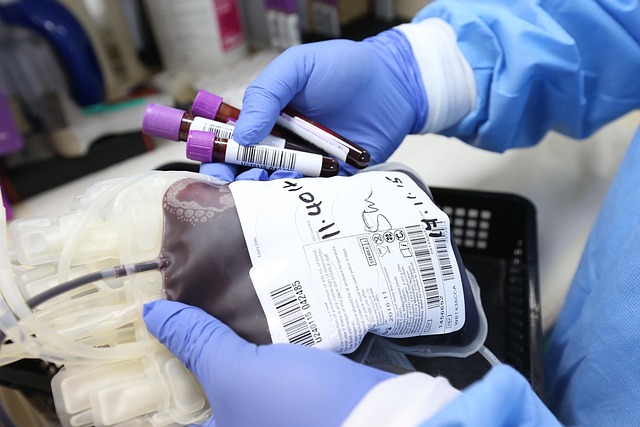
The bone marrow serves as the body’s blood cell factory, continuously producing red blood cells to carry oxygen, white blood cells to fight infection, and platelets to control bleeding. In myelodysplastic syndrome, genetic mutations disrupt this production process. The bone marrow may appear normal or even overly active under microscopic examination, but the cells produced are defective. These abnormal cells cannot perform their intended functions and often die prematurely. As healthy cells decline in number, the body struggles to maintain adequate oxygen delivery, immune defense, and blood clotting. The specific type of MDS determines which blood cell lines are most affected. Some forms primarily impact red blood cells, causing anemia, while others affect multiple cell types simultaneously. Over time, the accumulation of abnormal cells can crowd out healthy production entirely. In approximately one-third of cases, MDS progresses to acute myeloid leukemia, a more aggressive blood cancer. This progression risk varies depending on the specific MDS subtype and certain genetic markers. Regular monitoring through blood tests and bone marrow examinations helps healthcare providers track disease progression and adjust treatment strategies accordingly.
Living with myelodysplastic syndrome requires ongoing medical supervision and often involves treatments ranging from supportive care to more intensive interventions like chemotherapy or stem cell transplantation. The treatment approach depends on disease severity, patient age, overall health, and specific genetic characteristics of the abnormal cells. Supportive care may include blood transfusions to manage anemia, antibiotics to prevent or treat infections, and medications to stimulate blood cell production. Some patients benefit from drugs that modify disease progression. Early detection through recognition of subtle symptoms provides the best opportunity for effective management and improved quality of life.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.